Showing 100 Results
Filter By Date
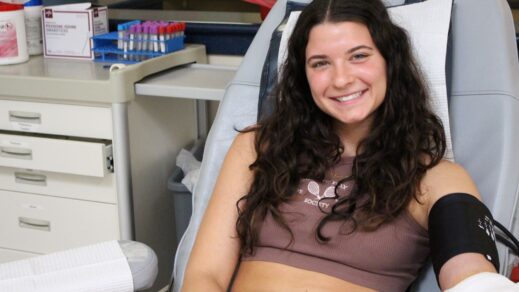
University of Delaware Connection to Blood Bank of Delmarva Remains Strong
Apr 22, 2024

Delaware Nepali Society Blood Drive brings in nearly 40 donors during blood emergency
Apr 18, 2024

New Castle County Government blood drive provides support for blood emergency
Apr 12, 2024
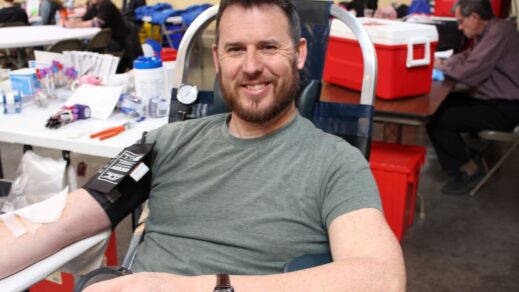
Every Drop Counts Blood Drive succeeds with 61 donors and support from the community
Apr 12, 2024

Blood Bank of Delmarva Declares Blood Emergency
Apr 8, 2024

3rd annual Out for Blood Drive set for April 20
Apr 1, 2024

March: A month of firsts for high school blood drives at BBD
Mar 27, 2024

Every Drop Counts Blood Drive honors Caleb Quick and his battle against childhood cancer
Mar 26, 2024
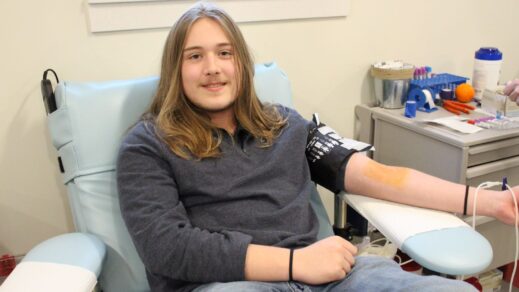
Benjamin Parsons joins the ranks of BBD 16-year-old donors, a new initiative
Mar 12, 2024

Blood Bank of Delmarva presents Dr. Charles Drew Lifesaver Award to William Garrett
Feb 29, 2024